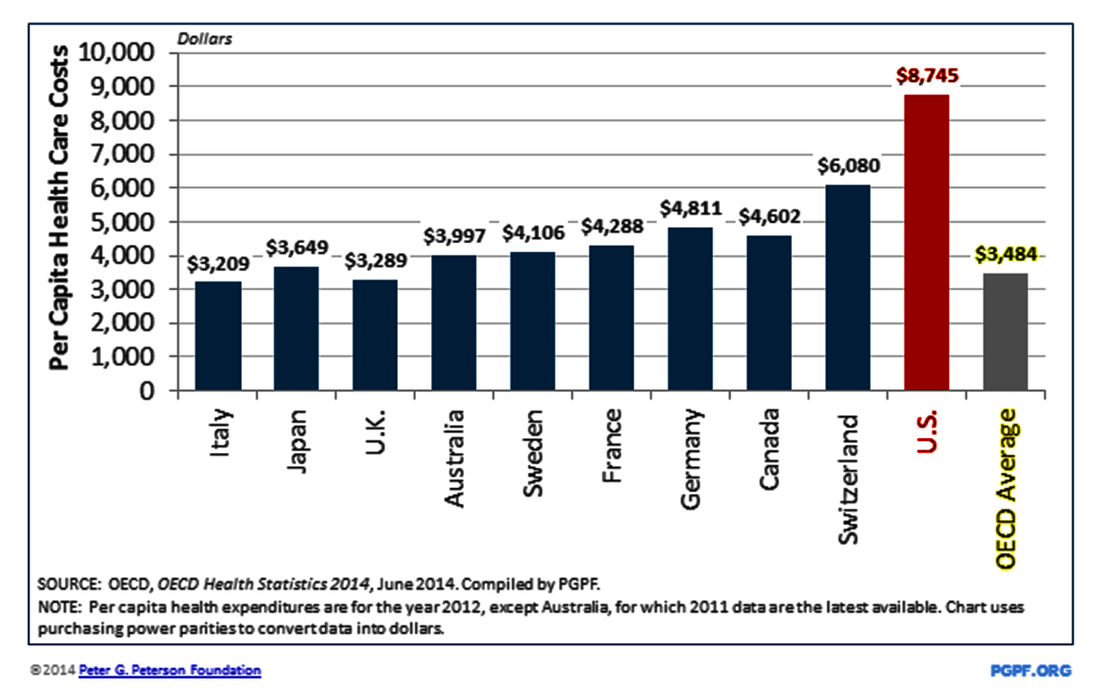
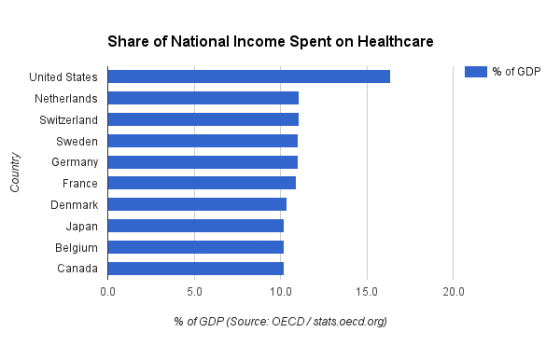
After all, these For-Profit Big Healthcare and Wall Street- and Washington-based “special interests” want to preserve a “marketplace- and monopoly-dictated healthcare patchwork” that saddles America with a world-leading and ever-spiraling $3.3 TRILLION in annual expenditures, gobbling up over 17 percent of our nation’s Gross Domestic Product (GDP). What this translates to is Americans paying about $9,000 per-capita for healthcare in the USA – almost 50-percent higher than the next highest nation (Switzerland) and about THREE TIMES more than the average ($3,484) among nine of the Organization for Economic Cooperation and Development (OECD) nations with Universal Healthcare systems listed in the bar chart below.
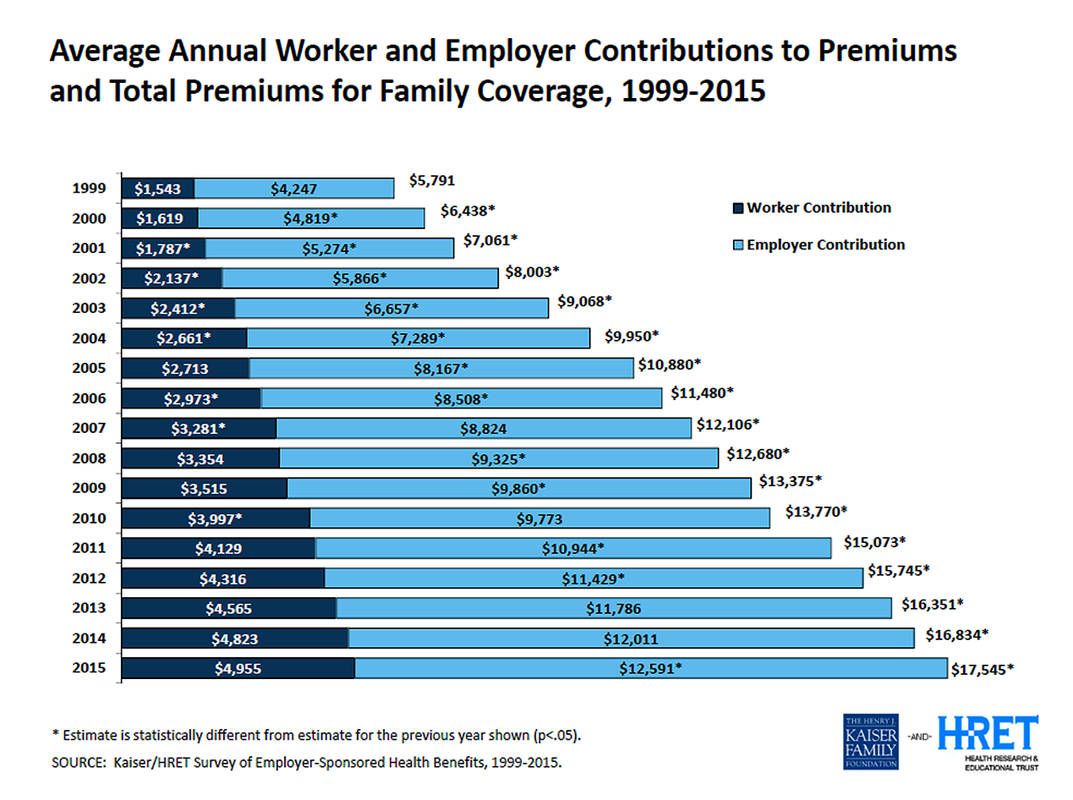
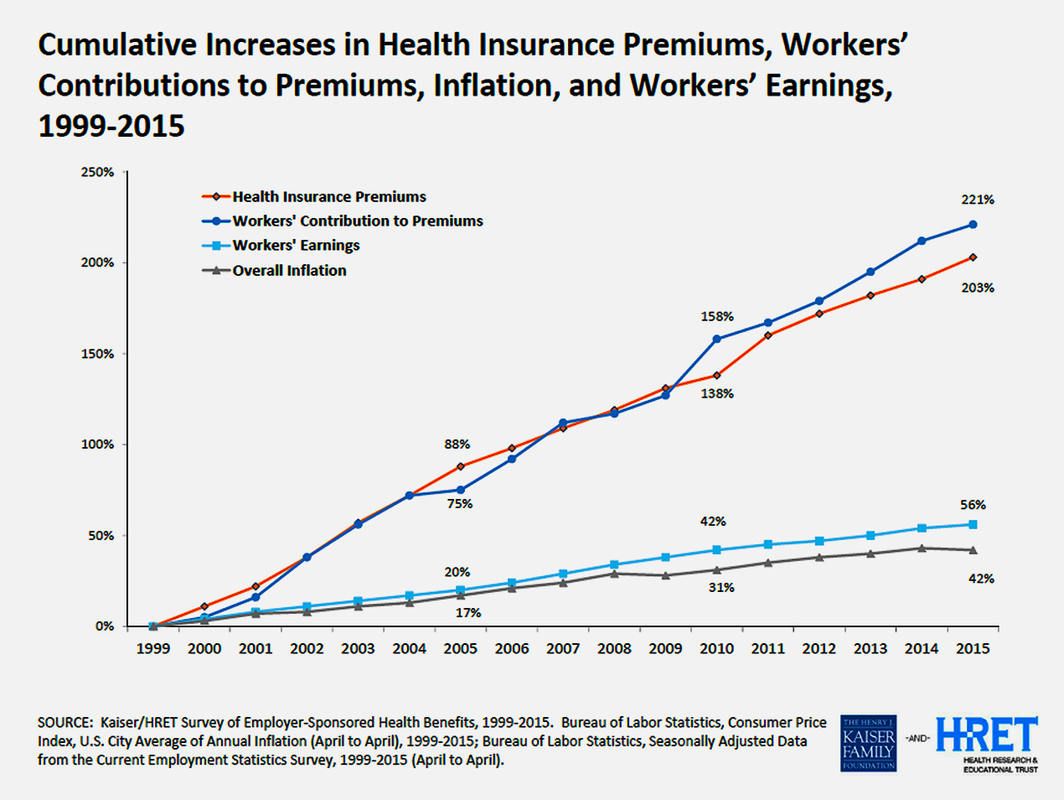
The $17,545 average for a “family” premium in 2015 represented a smaller 4-percent increase from the previous $16,834 average in 2014. But if you go back to 2010, when Congress had at first passed the Affordable Care Act into law, the average “family” health insurance premium came with a $13,770 average, followed by a 9 percent annual increase to $15,073. The first year of the Healthcare.gov and state-run exchanges in 2014 did slow annual growth to 4 percent from the 2013 average of $16,351. (It is also interesting to note that the total cost of a family premium in 1999 [$5,791] has risen a whopping 203-percent over the course of 16 years to $17,545 for 2015).
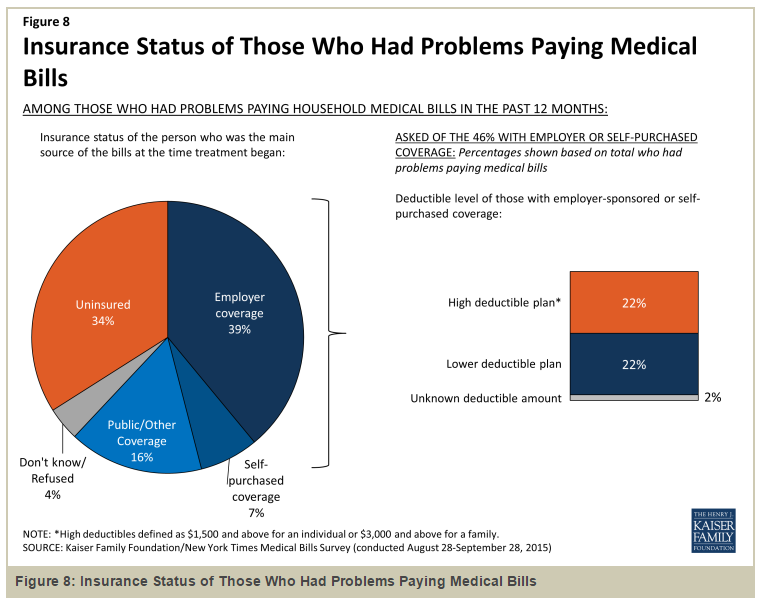
Whatever positve “halo effect” may be hoped from the enactment of the Affordable Care Act/Obamacare had no impact on how For-Profit/Big Health Insurers continued to somewhat more subversively shield “cost burden shifting onto the backs of American workers” in order for them to preserve and continue to grow certain levels of profitability for their “publicly-traded corporations” obsessively seeking to meet Wall Street “earnings expectations.” Most alarmingly the “burden-shifting strategy” employed by the For-Profit/Big Health Insurance monopolists not only centers on raising deductible levies on American consumers, it also applies to co-pay burdens additionally growing at an undocumented pace, too.
As the chart from ObamacareFacts.com lays out below, the ACA tax penalties started at $95 per-adult and up to $285 per-household levied on American taxpayers who did NOT file statements of proof with the Internal Revenue Service that they were in compliance with mandated health insurance coverage. In the most recently completed 2015 tax year, the individual penalties increased to $325 per-adult and up to $925 per-household fines. Starting in tax year 2016 in what U.S. Department of Health and Human Services (HHS) and U.S. Treasury Department have claimed will be a topped-out $695 per-adult and up to $2,085 per-household and will hold at that level for the foreseeable future.
The business cable TV network, CNBC, reported in July 2015 that 12 million Americans (those extensively rumored to be hovering between the 138- to 400-percent FPL) successfully received “exemptions” from the ACA mandate tax penalties. That represented 9-percent of all filers, reported CNBC, which noted earlier Congressional Budget Office projections were for upwards of 20-percent of all filers seeking “exemptions.”
Perhaps, most perplexing is CNBC reporting upwards of 5.1 million Americans “failed to state they had health coverage, or say they had paid the fine, citing unnamed “IRS officials.” The network reported that the IRS is now “analyzing these cases to determine their status,” according to a letter IRS officials sent to Congress.
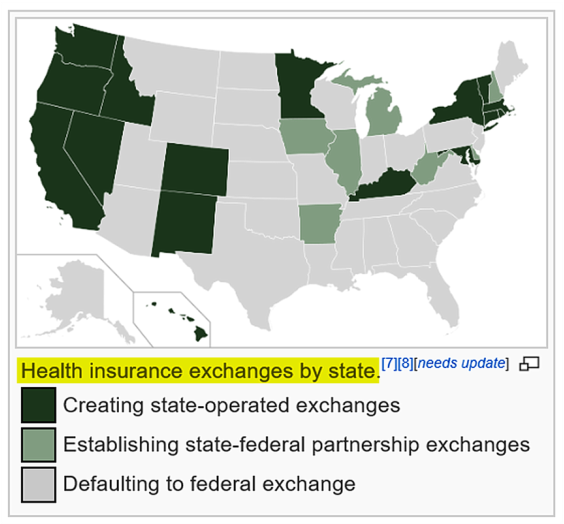
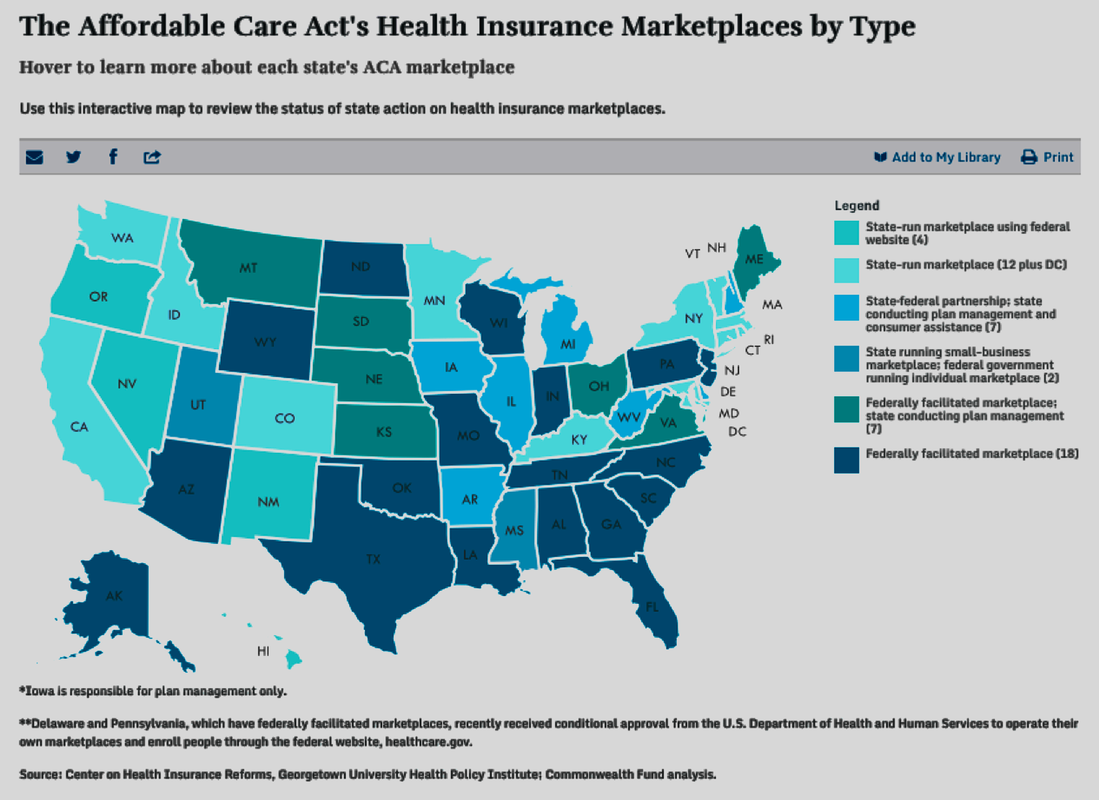
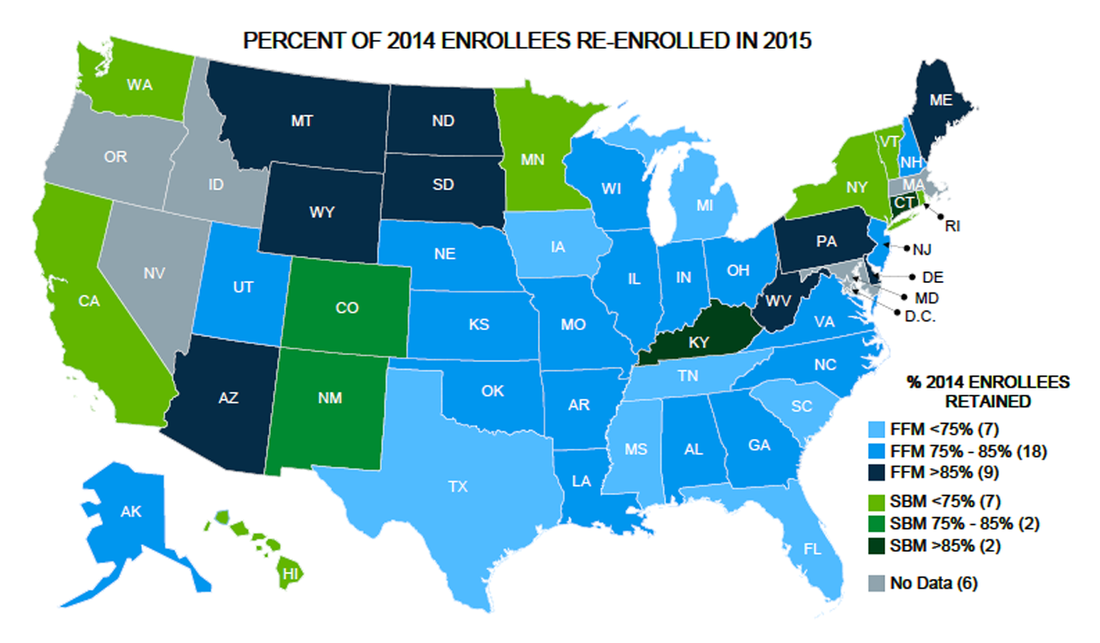
The cloudy status of some taxpayers who have potentially become Obamacare/ACA “mandate scofflaws” (in some cases) was originally the anticipated source and point of contention between the 27 states which filed to sue the federal government over the “Constitutionality” of “mandated” healthcare coverage. The number of states filing lawsuits also coincided with the states graphically depicted in the chart below (from Wikiepedia.org) which declined federal funding for creating “state-run insurance exchanges” (instead “defaulting” to the federally-run Healthcare.gov exchanges) and conversely refusing federal funding for expansions of Medicaid coverage for the poor-to-low-income Americans at the 138-percent and below Federal Poverty Line for coverage).
Not surprisingly, all but two of the remaining 27 states — those who sued the federal government over the “Constitutionality” of mandated health insurance and marketplace exchanges — instead refused state funding and participation, but nonetheless “defaulted” to the “federally-facilitated” Healthcare.gov national marketplace exchange web portal for their residents to choose from available participating health insurance plans.
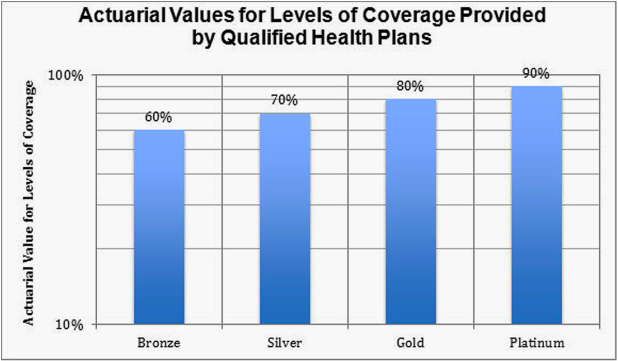
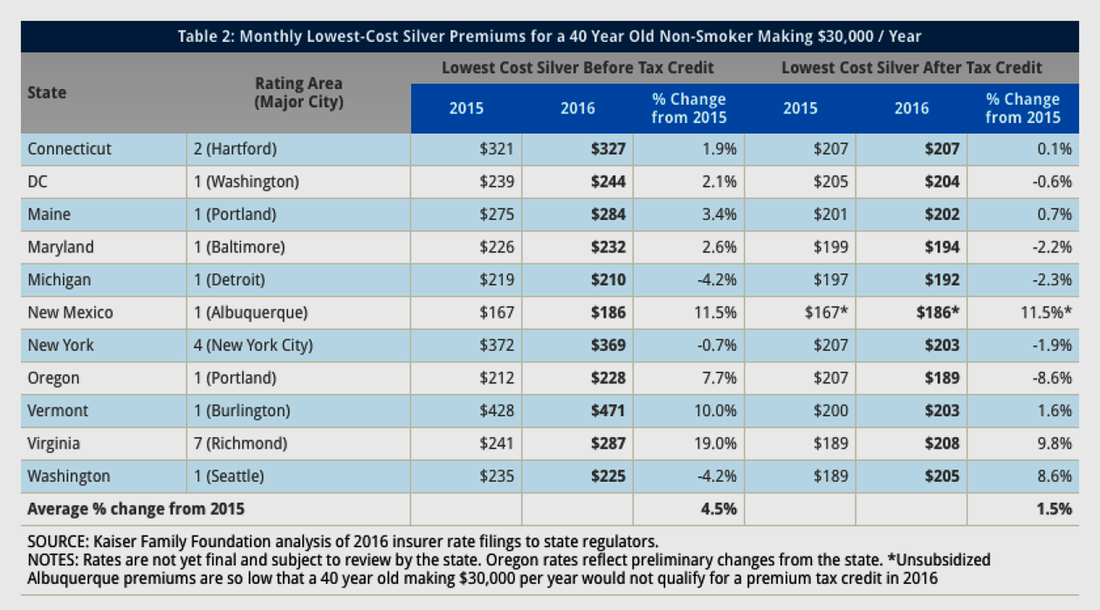
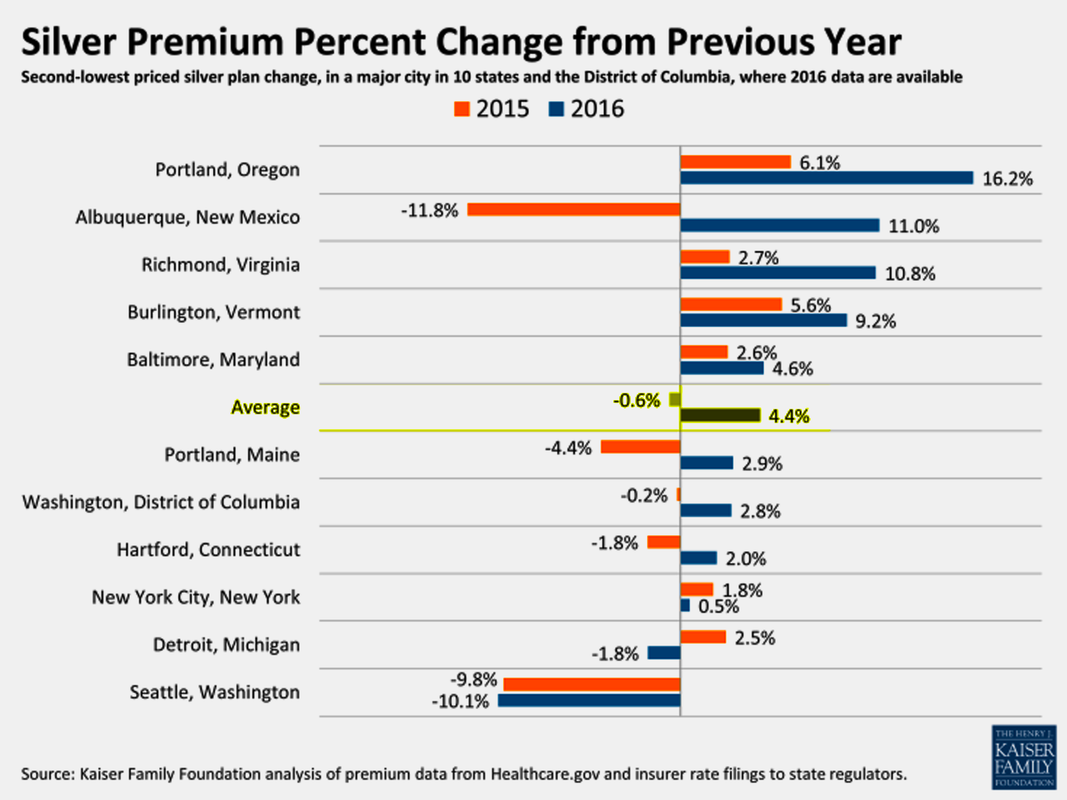
Across the 11 major metro areas, Burlington, Vermont came in on the high end at $471 per-month costs before federal tax credit while Detroit, Michigan and Albuquerque, New Mexico came in at lowest range $210 per-month (subsidized) and $186 per-month (unsubsidized) in 2016, respectively — keeping in mind that 70-percent actuarial level means the individual consumer will pay the other 30-percent of medical costs (not counting other deductible and co-pay costs, too).
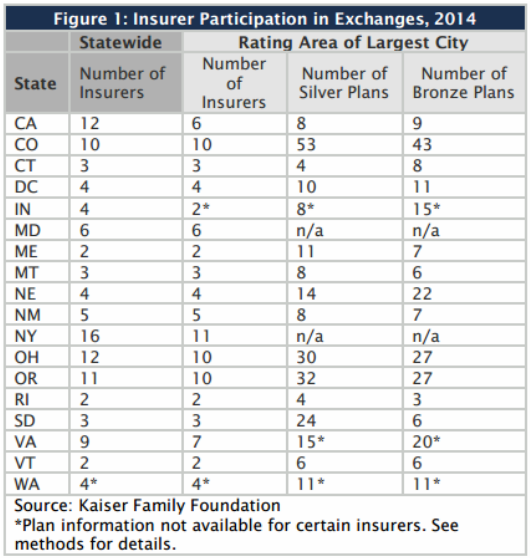
What’s most interesting is that 11 exchanges offered consumers premiums at an average $278 per-month charge for the “lowest cost” Silver plan before tax), a rise of 4.5-percent over the comparable 2015 average. After-tax credits from the federal government (based on several factors including income at 100- to 400-percent Federal Poverty Levels and the metallic level of insurance coverage), however, the “after tax credits” offer a roughly 28-percent credit to taxpayers, translating to a comparable $199 per-month premium average across the 11 exchanges and a smaller, adjusted 1.5-percent increase over 2015 for the comparable individual silver plan premium.
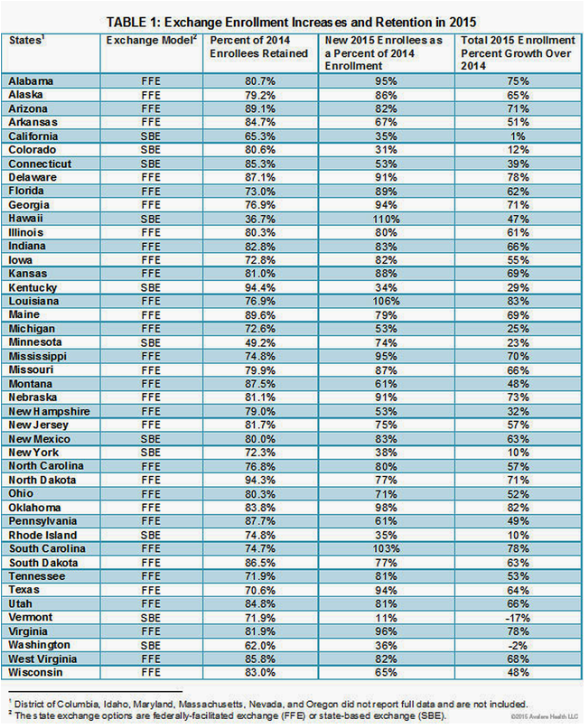
In the larger populations states like California, running Covered California as a SBE marketplace exchange, its first-year retention was 65.3-percent and second-year growth was just 1-percent for 2015. New York, also running an SBE, had just 72.3-percent retention and 10-percent growth. The two most populous states in the union most likely suffered the greater customer churn because consumers conversely have larger “private-market” health insurance and community health plan competition and choices by a relative margin over the lower population states.
Nevertheless, some Wall Street analysts have pegged some of Humana’s losses due “costs” associated with the ongoing Aetna merger process. However, Aetna has claimed to fare somewhat better financially in the ACA public exchanges and, in potentially absorbing what might be left of Humana’s exchange business, is said to be considering expanding its participation in some key state exchanges. Another For-Profit/Big Health Insurance carrier, Centene, completed a takeover of former competitor Health Net, which increases its presence in the ACA public exchanges and having it consider further expansion into other state marketplaces.
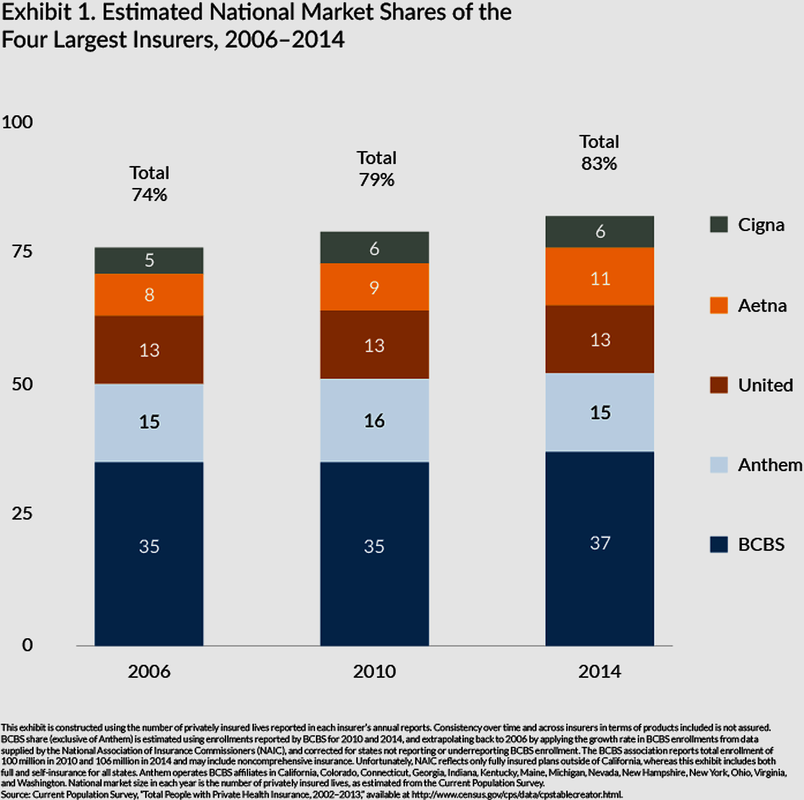
Anthem, a publicly-traded owner/operator of “for-profit-based” Blue Cross/Blue Shield franchises in 14 states, is also talking about some ACA public exchange plan expansions. Given that a handful of Big Health Insurance carriers hold a dominant 83-percent market share of the overall U.S. insurance marketplace, don’t expect any new choices and increased competition anytime soon.
The ruling will not have an immediate effect on the law because the judge put the decision on hold pending an expected appeal by the Obama administration. But it adds to uncertainty over the future of President Obama's signature domestic policy achievement ahead of the November 8, 2016 presidential and congressional elections, including whether enough health insurers will continue to participate in the ACA public exchanges.
The long-standing, entrenched nature of antitrust-exempt, monopoly-based “For-Profit/Big Health Insurance has also pretty much made it FREE of any federal regulation and oversight for the last THREE-QUARTERS of a century. That’s due in large part to Congress passing one of the most “unconstitutional” pieces of federal legislation, the McCarran-Ferguson Act of 1945, which essentially gives the Big Health Insurance Carriers an “exemption” from being regulated by the federal government (the feds leave it up to largely toothless “state insurance commissions” typically chaired and stocked with former For-Profit/Big Insurance executives to "regulate" them).
During the height of the largely “closed-door” Healthcare Reform debates in the Senate and House, Sen. Patrick Leahy (D-Vermont) and Rep. John Conyers (D-Michigan) both introduced and authored (in their respective houses of Congress) concurrent bills calling for the “repeal” of the McCarran-Ferguson Act. To the relief of consumer advocates, the House had voted affirmatively for its repeal. However, during the midnight hours on the eve of the Affordable Care Act’s passage, then-Senate Majority Leader Sen. Harry Reid (D-Nevada) had quietly announced that Leahy’s senate repeal bill had been “tabled for a lack of a quorum,” essentially a coded message that the For-Profit/Big Healthcare Lobby had gotten to a majority of the senators to ignore that effort. In all four bills seeking to repeal McCarron-Ferguson had been introduced to the House and Senate over the last 10 years (including by Conyers again in January 2015) – all of them meeting the typical “wall of silence and indifference” from a Congress, which refuses to live up its Constitutional oath of “Serving in the Public Trust.”
The passage of the Patient Protection and Affordable Care Act of 2010, however, did offer a few symbolic attempts in the federal legislation, somewhat briefly including the end of rescissions of health insurance policies and DENIAL of claims because of relatively higher costs associated with urgent-care surgical and elective medical procedures (some falling into the “experimental” category).
Nevertheless, there have been some widespread accounts that the For-Profit/Big Health Insurance monopolists are up to their old tricks on “denials of claims,” including USA Today reporting on a 37-year-old man with life-threatening cystic fibrosis who has difficulty with breathing, but his doctors recommended a new life-saving “breakthrough drug” called Kalydeco, which costs $25,000 per-month for prescription treatments. As it turns it, the man’s insurance carrier, UnitedHealth Group approved the medication for his sister (diagnosed for the same mutation of cystic fibrosis, but the brother is denied four times because the drug is “not FDA approved” at the moment (July 2013) and a UnitedHealth claim reviewer says his condition is NOT life-threatening while his sister’s same medical condition is deemed life-threatening.
A close friend of mine who also works in the “diagnostic” area of a family clinic has repeatedly related to me stories about how her clinic’s “at-risk” patients have been routinely denied claims to have certain Electrocardiogram (EKG), Magnetic Resonance Imaging (MRI) and CAT Scan (CT) diagnostic tests completed -- even though the patients received a doctors’ “pre-authorization” or “referral” to do the diagnostic procedure. It may be a more common practice because your claim might be denied by the Health Insurance Carrier if the a “pre-authorization” is lacking a formal doctor’s statement, which my friend said is sometimes still ignored by the health insurance provider.
Out of the passage of the sausage-made Affordable Care Act, it was thought the Big Health Insurance monopolists made a big concession regarding the industry’s stand on pre-existing conditions. But the bill has a giant loophole: insurers can continue to cancel policies in cases of alleged “fraud or intentional misrepresentation” by premium holders as they do now, according to Huffington Post’s report dating back to May 25, 2011. “Readers have no doubt hear of or read about how low the permitted bar is now for insurers to rescind policies. And when are insurers most likely to look to find grounds not to pay for treatment? When you most need it, of course, when you have a serious, expensive ailment,” HuffPo’s article noted.
There also other published reports like one in August 2014 from the Las Vegas Journal Review about a woman who gave premature birth to a daughter who still needed two subsequent surgeries and a 40-day stay at Summerlin Hospital there. Unfortunately, their health insurer, Blue Cross Blue Shield of Nevada cancelled their policy retroactively after the hospital had a “typo” on one of the claims listing the mother’s birthday as one year earlier – with BCBS citing the intentional misrepresentation and fraud provision in getting out of the daughter’s surgeries and extended hospital stay.
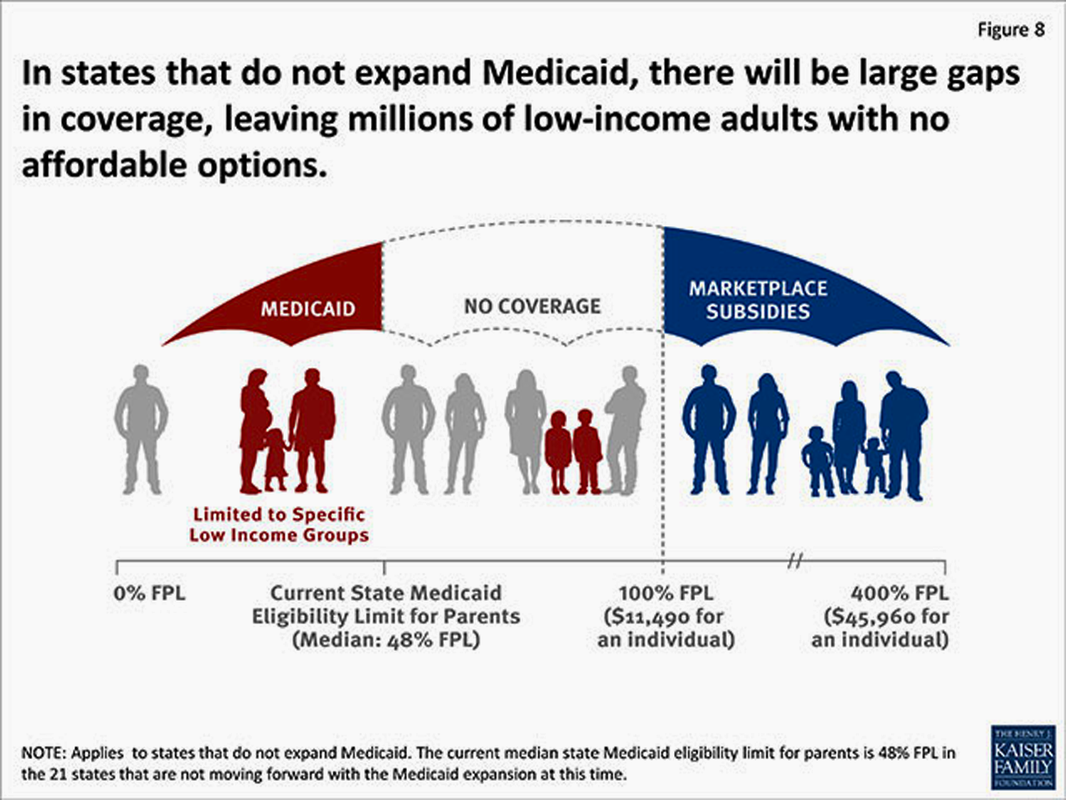
The Huffington Post account in “An Inglorious End to the Promise of Reform” best summed up the “Catch-22” nature of the ACA’s “individual mandate” on obtaining healthcare in America: “Individual mandate was the top priority of the insurance industry, which also succeeded in fending off meaningful restraints of its predatory pricing practices. The likely outcome is that far too many people will still face health care insecurity or medical bankruptcy due to ever rising out-of-pocket costs, or continue to skip needed medical care because of the high prices. Indeed, discouraging provision of care as the preferred way to control costs, rather than rein in the pricing practices of the insurance and drug giants, is a central tenet of the insurance industry and conservative policy wonk.”
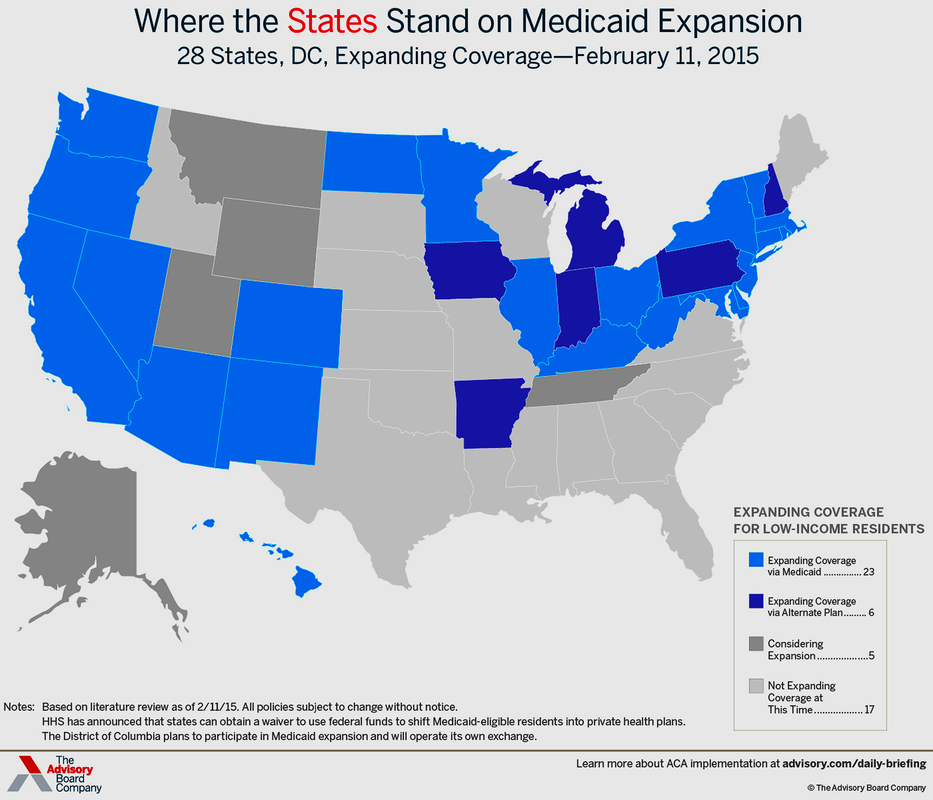
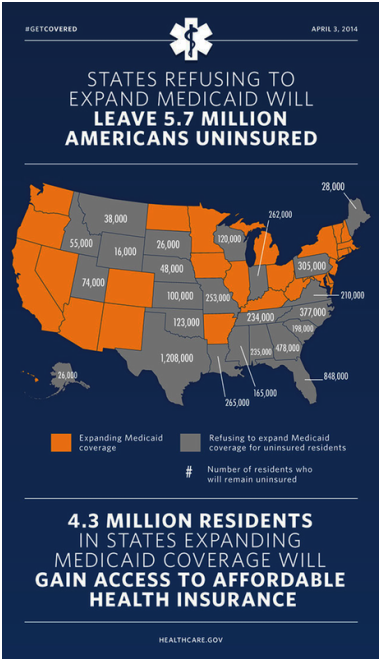
In fact, largely coinciding with how Republican-led “Red States” had already refused to join the ACA/Obamacare public exchanges with “state funding and operational participation,” these are mainly the states also refusing to expand Medicaid plan offerings (even though it is federally funded) to lower-income to indigent individuals and families falling within 138-percent of the Federal Poverty Line. As the Advisory Board Company map below illustrates, 22 of the mostly Southern and Plains states declining to participate in the Medicaid Expansion, five of the darker gray-colored states are “considering expansion,” but 17 of the lighter gray states are “not expanding coverage” at this time (dating back to February 11, 2015).
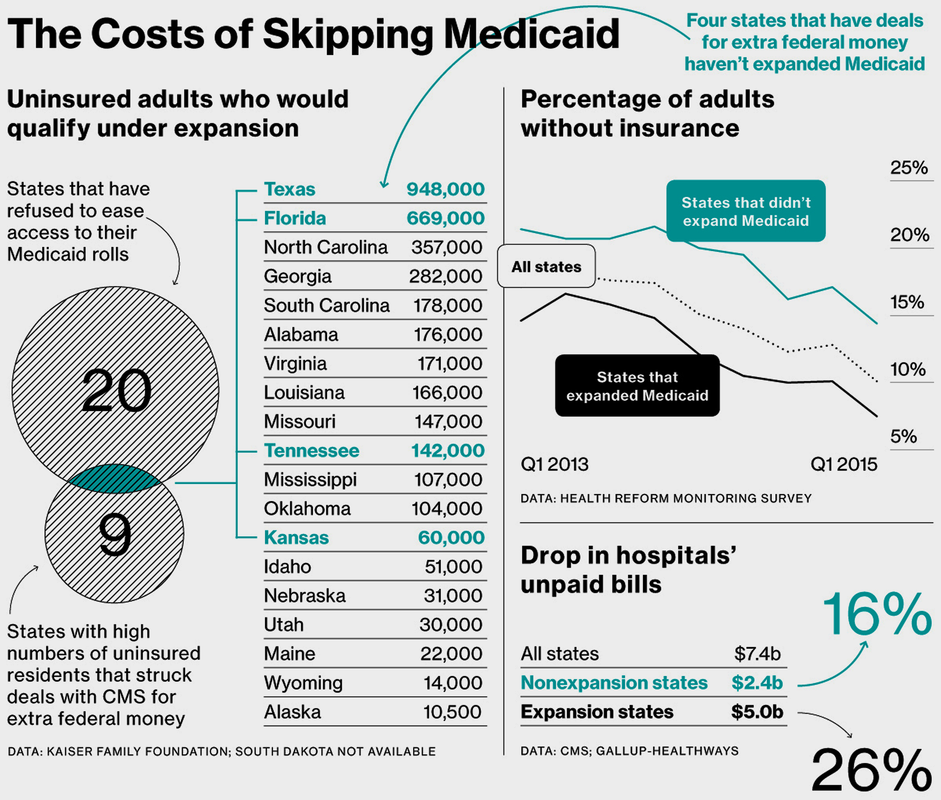
Florida and Texas are among nine states with high numbers of uninsured residents that struck deals with CMS for extra federal money to help hospitals, which are legally bound to provide care whether or not patients can pay. The arrangements, known as “uncompensated care pools,” are subject to periodic renewal and were also granted to Arizona, California, Hawaii, Kansas, Massachusetts, New Mexico, and Tennessee. Of those, only Kansas and Tennessee have joined Florida and Texas in continuing to resist Medicaid expansion.
Florida is the first to come up for review since the Affordable Care Act went into force. Florida Governor Rick Scott, a Tea Party conservative, opposed expanding Medicaid when he took office in 2011, then reversed himself in 2013, saying in a news conference that with Washington picking up the tab, “I cannot, in good conscience, deny Floridians the needed access to health care.” With his state legislature dominated by conservative Republicans, he wavered.
The “grandfathered” federal funding from CMS has allowed the four holdout states – Texas, Florida, Tennessee and Kansas – to reduce the number of uninsured residents of their states and similarly benefit, along with the “Medicaid expansion states,” to see that their states’ “uncompensated care pools” receive the federal funding to reduce hospital costs by $5 BILLION by the first quarter of 2015.
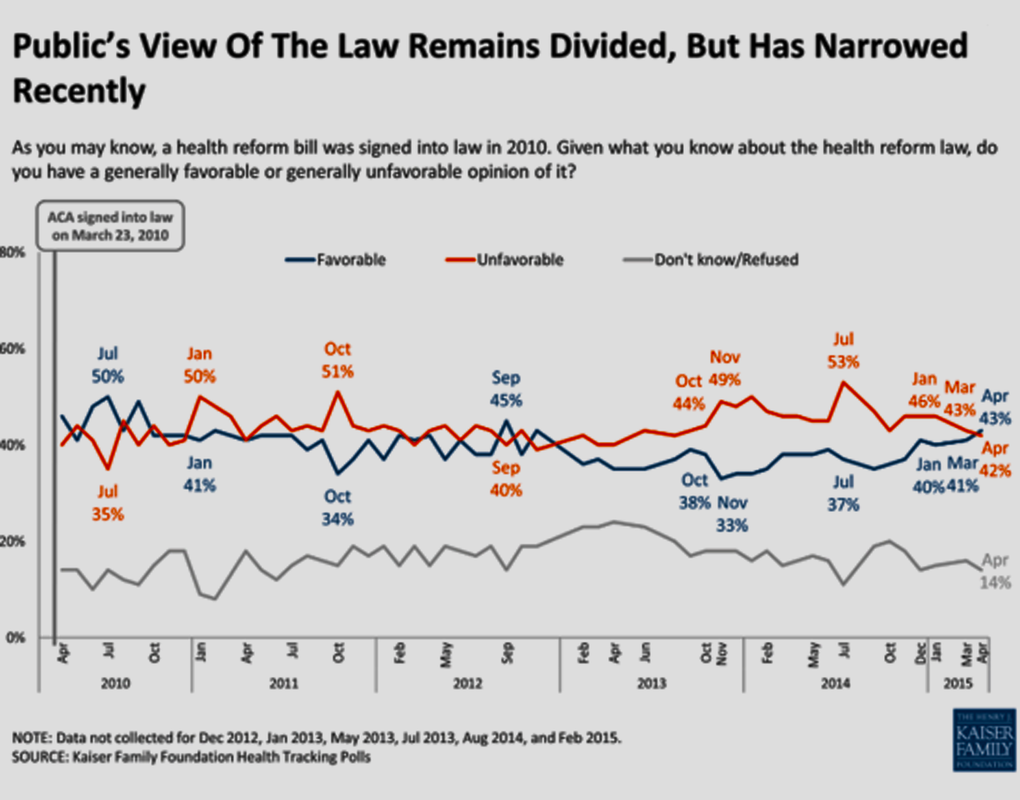
The American public remains the most telling barometer on Obamacare’s success and long-term viability, though. Like the states remaining divided on accepting or fighting “mandated” health coverage, the American public, according to Kaiser Family Foundation Health Tracking Polls (in the five-year poll of 2010-2015 attached below), remain almost evenly divided, but the trend line for Americans viewing Obamacare “favorably” rose from 37-percent in July 2014 to 43-percent in April 2015.
Most notably, the split in American public opinion on Obamacare is, perhaps, emblematic of the teetering nature of its potential to lose continued federal funding, especially if Republicans grab the White House and continue to hold majorities in both houses of Congress by January 2017. Outside of the great “external threats” politically for the Affordable Care Act facing a “successful” repeal vote in Congress, the inherent, ever-escalating “price-gouging increases” successfully engineered by the antitrust-exempt “For-Profit/Big Health Insurance” monopolists challenges the basic financial underpinnings of the ACA public insurance exchanges as well as the open “commercial marketplace” for both individual and family premium consumers.
Lastly, the number of states (20 or more) continuing to refuse to participate on state-level contributions to the expansion of Medicaid to provide subsidized health coverage for low-income/indigent Americans by suing the federal government over the Constitutionality of “mandated” health insurance coverage, is creating an ever-widening Grand Canyon-sized chasm for the ACA-participating states and federal government to continue “bridging.” It is still an inescapable fact that approximately 22 million Americans remain “uninsured” and “uncovered” when it comes to either needing urgent care treatment for a catastrophic illness or accident – leaving them in dire fear of ever facing such an event.
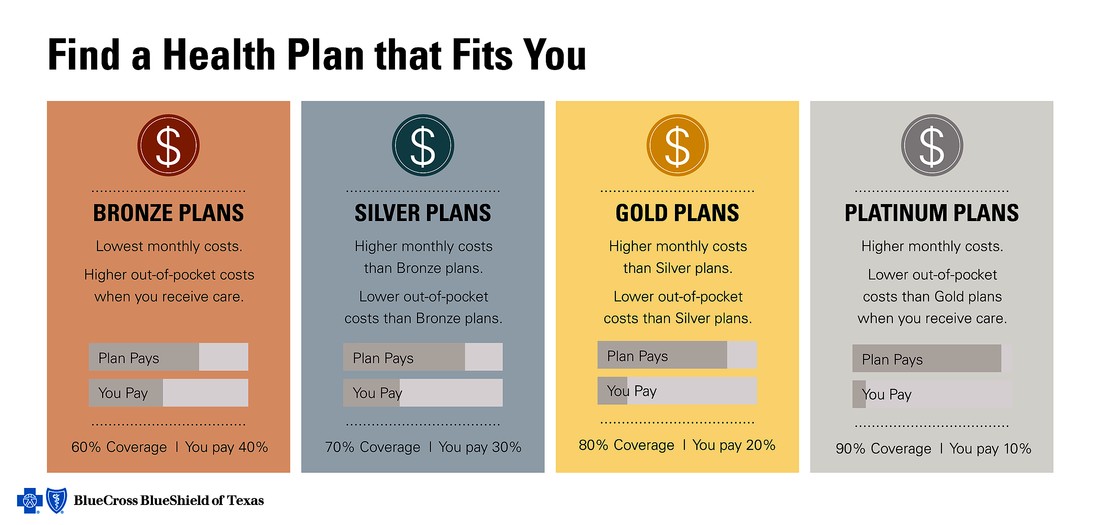
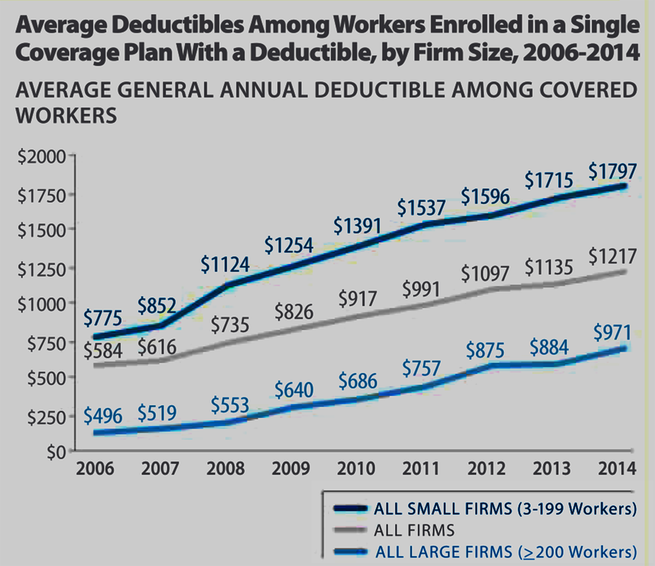
For the Americans who can either afford costly, artificially-inflated health coverage (remember the KFF research listed above, citing a 200 percent-plus increase in insurance premium costs from 1999 to 2015!) from the For-Profit/Big Health Insurance or qualify for tax credits and subsidies to buy slightly lower-cost plan coverage through the ACA public exchanges, they are still faced with ever-increasing, burden-shifting higher out-of-pocket DEDUCTIBLES and Co-Pay expenses laden onto their shoulders. Even the specter of facing “tax penalties” for NOT being in compliance with ‘mandated” health insurance coverage pales in comparison with the overriding fear of personal bankruptcy due to overwhelming, partially or fully “uncovered” medical costs that weighs heavily on most Americans’ psyches…every day of their lives.
Back in March 2010, nearing the final House and Senate congressional votes for the Affordable Care Act’s extremely narrow, partisan passage, one of the lone Democratic holdouts, then-Rep. Dennis Kuccinich (D-Ohio), was famously quoted during his long holdout, suggesting Obamacare’s blueprint was akin to “building a foundation on quicksand.” (Kuccinich had been a long-time advocate of a broader “Single-Payer Universal Healthcare” system.)
Well, the house is still standing, but all of the economic and political indicators suggest that the ACA/Obamacare’s current foundation is showing some cracks/fissures and badly in need of massive repairs or a Herculean-type overhaul if it is going to survive well into the next presidency and session of Congress starting in January 2017. #
– Michael A. Freeman











 RSS Feed
RSS Feed
